Why Your Vascular Connection Matters
When starting hemodialysis, the connection between your blood and the machine is everything. This connection point, known as Dialysis Access, is the vascular method used to safely move blood out of the body and back in for cleaning. Without a reliable connection, treatments cannot happen effectively. Many patients don't realize how much choice exists until they are already in the waiting room. You generally have three paths to choose from, each with its own timeline and risks.
Think of these access points like doors. One door might be sturdy metal built from your own body parts, another uses synthetic materials, and the third is a temporary tube. Which one fits your life depends heavily on your veins, your overall health, and how quickly treatment needs to start. Getting the right one is crucial because some options carry higher risks of infection or clotting over time. We will walk through the specifics so you know what to ask your doctor during your next appointment.
The Preferred Choice: Arteriovenous Fistulas
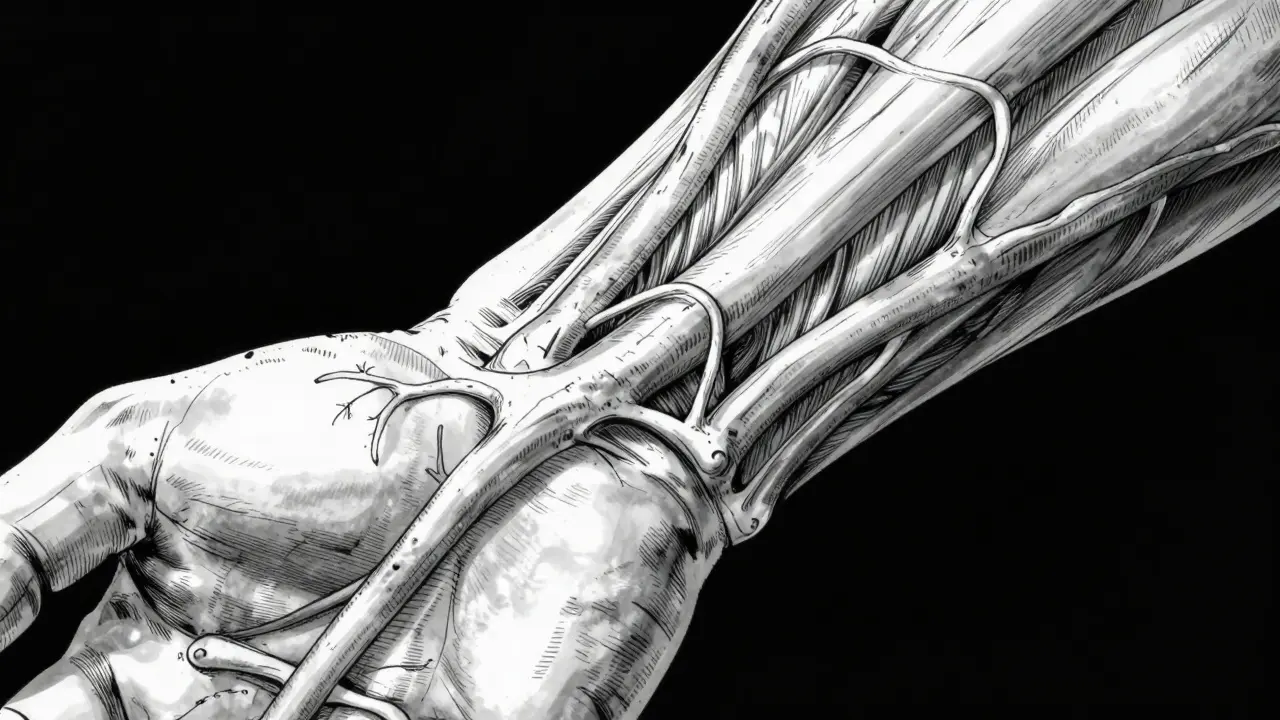
If you can get one, an arteriovenous fistula is usually the best bet. A AV FistulaArteriovenous Fistula is a surgically created connection between an artery and a vein in your arm. Doctors perform this procedure by linking the two vessels directly. Once connected, the high pressure from the artery flows into the vein. This forces the vein to thicken and grow stronger over time, turning it into a robust channel capable of handling heavy needle traffic.
This is considered the gold standard by major organizations like the National Kidney Foundation. Their guidelines recommend it for almost everyone starting treatment. Why? Because your own tissue heals better and fights infection more effectively than foreign materials. A well-made fistula can last decades. Some patients keep their original access working perfectly for over ten years with just routine check-ups.
However, patience is required here. After the surgery, you cannot use it immediately. The vessel needs to "mature." This process typically takes between 6 and 8 weeks. During this time, you need to monitor the site daily. You should feel for a vibration, often called a "thrill," which signals blood is flowing freely. If the thrill disappears, that's a warning sign something has clotted.
Synthetic Bridges: Arteriovenous Grafts
Not everyone has veins strong enough for a fistula. Sometimes the arteries and veins aren't accessible or healthy enough. In those cases, doctors turn to an Arteriovenous Graft, a synthetic tube made from biocompatible material connecting an artery and a vein. This acts as a bridge when your natural vessels won't work alone.
The biggest advantage of a graft is speed. While a fistula needs months to mature, a graft is usually ready for use in just 2 to 3 weeks. This matters if you need to start treatment sooner rather than later. The material is typically polytetrafluoroethylene, a soft plastic designed to sit under your skin without rejecting easily.
Despite the convenience, grafts come with higher maintenance needs. They are more prone to clotting than fistulas. Statistics suggest that roughly 30% to 50% of grafts will require some kind of intervention within the first year to stay open. This might mean going back to the hospital for a minor procedure to clear the clot. They also tend to have a shorter lifespan, often needing replacement after 2 to 3 years. If you choose a graft, you must attend all follow-up appointments to ensure it stays patent.
Temporary Measures: Central Venous Catheters
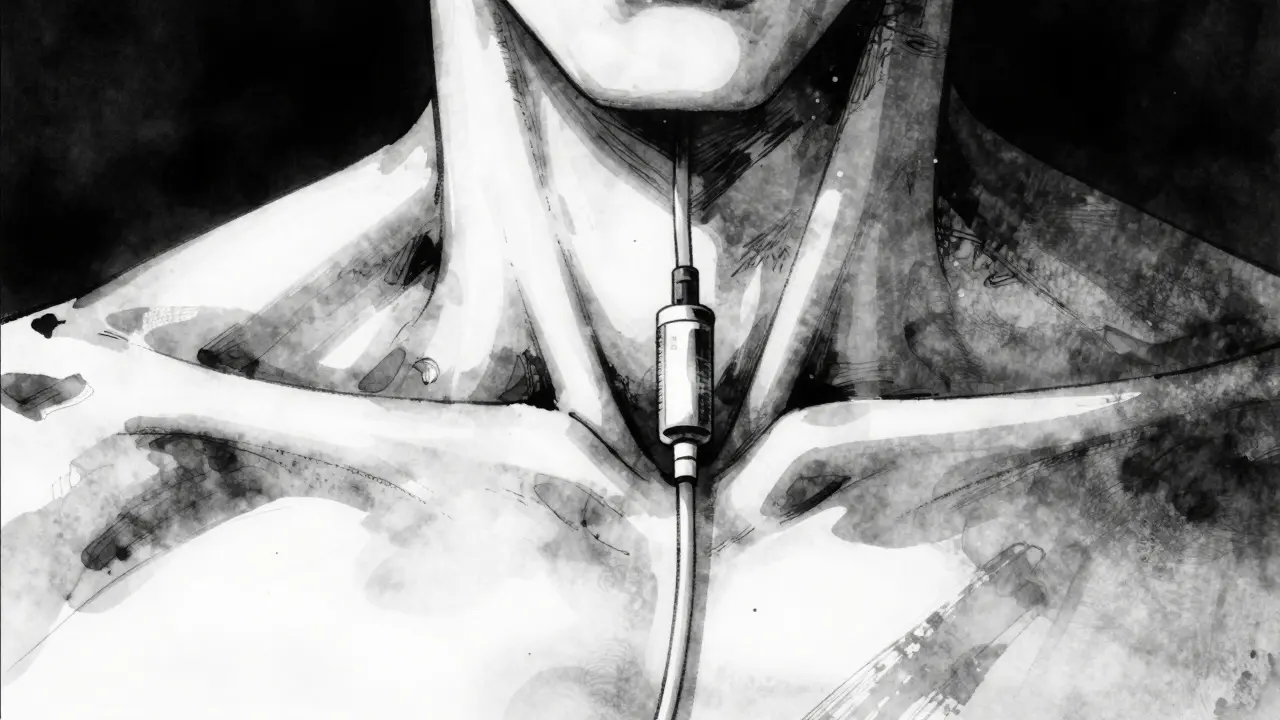
Sometimes, permanent options aren't immediate. A Central Venous Catheter is a soft tube placed into a large vein in the neck, chest, or groin for immediate access. These are meant to be temporary solutions until a fistula or graft heals. However, some patients end up relying on them permanently because other access isn't feasible.
Care for this type of access is intensive. Because the tube sits partly outside your body, it creates a direct path for bacteria to enter your bloodstream. Keeping the area dry is non-negotiable. Bathing becomes tricky; you cannot soak the exit site in water. Showering requires a waterproof covering, and even then, there is risk. Most centers recommend sponge baths for the area around the catheter.
Infection rates are significantly higher with catheters compared to other methods. According to recent clinical reviews, patients with catheters face a substantially higher risk of fatal infections than those with fistulas. While convenient to place, the long-term health trade-offs are steep. Ideally, a catheter is a bridge, not a destination. If you find yourself stuck with a catheter for a long time, you need to be extra vigilant about hygiene and reporting any fever or redness immediately.
Understanding the Risks and Numbers
You might wonder if the difference between these options actually impacts survival. The data is clear and quite stark. Studies comparing different access types show significant differences in outcomes. Research published in medical databases indicates that using a catheter versus a fistula is associated with a 1.53 times higher risk of mortality. That represents roughly 106 excess deaths per 100,000 patient-years.
Grafts sit somewhere in the middle. The risk is lower than catheters but still higher than fistulas. Even with grafts, there is a noticeable increase in clotting events. In terms of infections, the gap is even wider. Fatal infection risks are 2.12 times higher with catheters compared to fistulas. This statistical reality is why the "Fistula First" initiative was launched decades ago-to encourage moving patients toward the safest option whenever possible.
| Feature | Arteriovenous Fistula | Arteriovenous Graft | Central Venous Catheter |
|---|---|---|---|
| Maturation Time | 6 to 8 weeks | 2 to 3 weeks | Immediate |
| Infection Risk | Lowest | Moderate | Highest |
| Average Lifespan | Years to Decades | 2 to 3 Years | Temporary |
| Intervention Rate | Routine monitoring | 30-50% need help | High maintenance |
Daily Care and What to Watch For
Once you have your **dialysis access**, your job is to protect it. For a fistula or graft, checking the site daily is part of your routine. Lie down and use your fingertips to feel for that vibration we mentioned earlier. It should feel like a hum or a buzz. If it stops, contact your care team immediately. Do not wait until your next scheduled session.
Keep the area clean, but avoid scrubbing too hard. Do not carry heavy bags on the arm with the access. Do not allow blood pressure cuffs to be placed on that arm. Even tight sleeves can compress the blood flow. Nurses can teach you how to check for swelling or skin color changes. Signs of infection include redness, warmth, or discharge. If you develop a sudden fever or chills, assume it could be related to your access.
Education makes a huge difference here. Patients who receive comprehensive pre-surgical education report fewer complications. Knowing exactly what normal looks like saves lives. You want to build a habit where you inspect the site every morning. It takes less than a minute, but it catches problems early when they are easier to fix.
Future Technology and Trends
The landscape is changing as we move into 2026. New tools are making management easier. Wireless sensors are now approved to monitor blood flow in fistulas automatically. Instead of you guessing if blood is flowing, a device can alert you if the flow drops below safe levels. Early trials showed a reduction in clotting events when these alerts were used consistently.
We are also seeing improvements in how surgeons create connections. Preoperative exercise programs can actually increase the chance of a fistula maturing successfully. This means doing specific exercises under guidance before the surgery to prepare the veins. Bioengineered vessels are entering trials too, offering hope for patients who have exhausted their natural vessel options. As the population ages and diabetes rates rise, these innovations become critical to maintaining quality of life for thousands of patients.
Can I switch from a catheter to a fistula?
Yes, if your blood vessels allow it. Switching reduces infection risk and improves longevity. Talk to your nephrologist about vein mapping to see if you are eligible for a permanent solution.
How often should I check my access site?
You should check it daily. Feel for the thrill or vibration to ensure blood is flowing properly. Look for redness, swelling, or leaks around the needles after treatment.
What are the signs of a blocked fistula?
The most common sign is the loss of the thrill. You might also notice swelling in the hand or arm. Immediate medical attention is needed to prevent permanent damage.
Does insurance cover vein mapping?
Most Medicare plans and private insurances cover vein mapping since it helps determine the best surgical plan. Confirm with your provider before scheduling the ultrasound exam.
How long does a graft last on average?
On average, grafts last 2 to 3 years before they may need replacement. Regular surveillance is essential to catch narrowing or clotting issues before they fail completely.




9 Comments
Kendell Callaway Mooney
March 31, 2026 AT 19:05 PMHaving worked in nephrology for years I can confirm that early planning saves lives. Many folks wait until their veins get damaged before considering the fistula option. Synthetic grafts often fail faster than native tissue connections. You need to understand your own vascular mapping before the crisis hits. Waiting too long means you end up stuck with a catheter which invites infection risks daily. Patience during creation allows the blood flow to mature properly over weeks or months. Rushing into surgery without proper assessment leads to complications down the road. Always consult a vascular surgeon specifically trained in access placement procedures. Family support plays a massive role in healing recovery periods too. Don't ignore the warning signs of restricted flow either.
Charles Rogers
April 1, 2026 AT 14:52 PMPeople think they know what works best for their kidneys without listening to medical professionals. This is dangerous thinking that puts entire households at unnecessary risk every single day. A fistula requires dedication and patience that most modern individuals simply do not possess anymore. They want quick fixes like catheters that offer temporary relief instead of longevity. Infection rates spike significantly when people bypass the recommended surgical pathways entirely. You might think convenience outweighs health outcomes but statistics prove otherwise quite heavily. Clotting issues arise frequently in those who neglect regular monitoring schedules after surgery. Negligence on part of the patient often leads to hospital readmissions within the first month. It is frustrating to see educated adults dismiss vital preparation steps for their own treatments. We lose potential life years because of these preventable complications occurring repeatedly. Education is lacking among patients who refuse to research their options beforehand thoroughly enough. Doctors spend hours explaining risks yet families still choose the easy path initially. Convenience breeds complacency which eventually results in severe cardiovascular strain later on. Ignorance regarding vein quality causes surgeries to fail before dialysis even begins effectively. We must hold ourselves accountable for asking better questions at appointments consistently always. Safety must be the absolute priority in all medical decision making processes.
Dan Stoof
April 2, 2026 AT 11:30 AMOh my goodness! That really drives the point home!! Your passion is evident!!! And it is absolutely necessary!!! We cannot ignore the facts!!! Safety comes first!!! Always!!! Every choice matters!!! Keep fighting!!! Stay strong!!! Never give up!!! Hope remains!!!
Cameron Redic
April 2, 2026 AT 14:48 PMEveryone knows catheters are worse but people panic and pick them anyway. It is pathetic how much information is out there yet ignorance wins. Stop relying on others to fix your mess when you ignored the signs.
Adryan Brown
April 4, 2026 AT 03:03 AMWhile I understand frustration arises during difficult health journeys we must remember everyone faces different challenges individually. Medical advice varies based on anatomy and personal history which dictates specific treatment plans uniquely for each person involved. Aggression rarely helps anyone improve their situation constructively moving forward through tough times. We should focus on supporting each other rather than assigning blame for choices made under pressure. Empathy allows us to grow together while facing chronic conditions alongside our community. Understanding different perspectives helps reduce conflict within groups discussing serious health topics online today. It takes courage to share stories and listen to experiences shared by strangers here freely. We build bridges instead of walls when we speak kindly about sensitive medical decisions privately. Everyone deserves compassion when navigating complex healthcare systems designed to preserve life primarily. Peaceful dialogue fosters healing environments where true learning happens naturally over time without hostility.
Biraju Shah
April 4, 2026 AT 18:57 PMYou guys need to wake up before your kidneys shut down completely. Wasting time on debates doesn't fix your plumbing problems inside your body right now. Get to the doctor immediately and demand the best connection possible today. Delays cost lives and nobody likes being told they were careless about their future. Stop reading threads and start getting checked up by actual specialists professionally. Hesitation kills more people than the disease itself ever does. Take charge of your health status before it is too late for action.
Jonathan Alexander
April 5, 2026 AT 12:13 PMThat is incredibly harsh for someone who clearly cares about helping others deeply though. Maybe tone down the urgency slightly so people don't feel attacked while reading. Stress adds nothing positive to the recovery process anyone goes through during diagnosis phases. We are all scared and sometimes fear makes us react poorly to advice given seriously. Please try to keep things constructive instead of demanding immediate action publicly like that.
William Rhodes
April 6, 2026 AT 16:14 PMEvery challenge presents an opportunity for growth in ways we cannot foresee initially. Choosing the right access opens doors to living fuller lives despite limitations. Positivity fuels resilience needed for long term treatment success stories everywhere. Believe in your capacity to heal and adapt to new routines successfully always. Light exists even in the darkest hospital rooms guiding us forward daily. Trust the journey ahead holds promise beyond current struggles we face right now.
Marwood Construction
April 7, 2026 AT 14:17 PMThe clinical guidelines suggest prioritizing fistulas whenever vascular anatomy permits successful creation.